New Guidelines Inform Diverticulitis Treatment
January 18, 2021
Treatment moves toward less use of antibiotics, less emphasis on surgery
Innovations in Digestive Health | Winter 2021
Colonic diverticulitis remains a painful, unpredictable gastrointestinal disease that can lead to serious complications, chronic symptoms and poor quality of life. While complicated cases require aggressive treatment, recent American Gastroenterological Association (AGA) guidelines suggest a more conservative approach for uncomplicated, nonsevere diverticulitis. Guidelines from the American Society of Colon and Rectal Surgeons (ASCRS) echo AGA’s recommendations.
 Trevor Teetor, MD
Trevor Teetor, MDIn light of these updated guidelines, University Hospitals Digestive Disease Institute has modified its approach to ensure patients receive the most up-to-date, comprehensive care possible. “The AGA guidelines reinforce the need for personalized care,” says Trevor Teetor, MD, colorectal surgeon and assistant professor of Colon and Rectal Surgery at Case Western Reserve University School of Medicine. “They will influence my prescribing style and approach to surgery.”
One notable change: AGA recommends selective, rather than routine, antibiotic use in immunocompetent patients with mild disease. “While antibiotics have long been first-line therapy for acute uncomplicated diverticulitis, recent evidence suggests there is no benefit in immunocompetent patients with mild acute uncomplicated diverticulitis,” the report states.
“We always thought acute cases involved an immediate infection,” Dr. Teetor says. “Now we understand it involves inflammation, which does not necessarily need antibiotics.”
AGA does, however, advise antibiotic treatment for patients with comorbidities, who present with concerning, high-risk symptoms or who present with complicated diverticulitis.
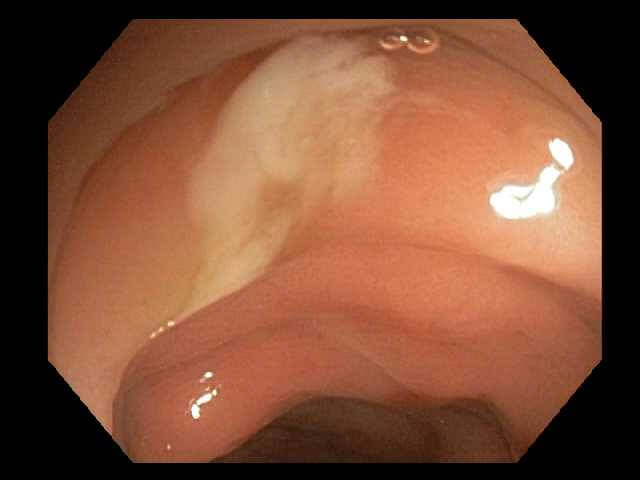 Caption: Pus in the inflamed segment of bowel is typical of diverticulitis.
Caption: Pus in the inflamed segment of bowel is typical of diverticulitis.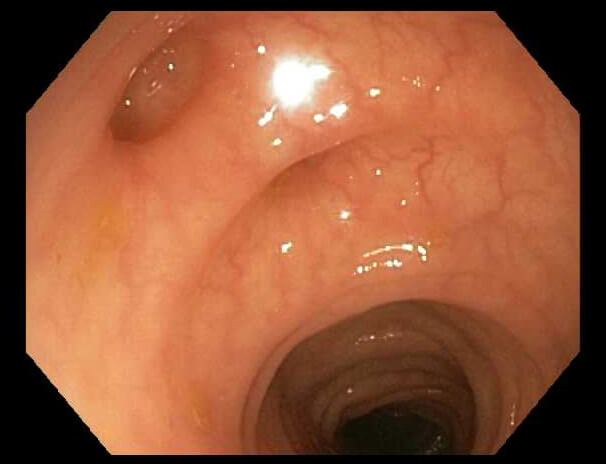 Caption: “Pouches” that form in the colon wall is typical of diverticulosis.
Caption: “Pouches” that form in the colon wall is typical of diverticulosis. A CONSERVATIVE APPROACH TO SURGERY
Guidelines around surgery have also changed. Surgeons should advise elective segmental resection on a case-by-case basis rather than on a specific number of episodes. Factors to consider include disease severity, patient preferences and values, and the benefits and risks. Chronic gastrointestinal symptoms may not improve with surgery.
The report states that at five-year follow up, patients with recurrent diverticulitis experienced improved quality of life after elective resection. However, 15 percent of patients experienced recurrent diverticulitis after surgery, and between 22 and 25 percent had ongoing abdominal pain.
POST-EPISODE COLONOSCOPY
Because the risk of malignancy is low, AGA recommends colonoscopy on a case-by-case basis. Colonoscopy is advised after complicated diverticulitis and after an initial episode. For recurrent, uncomplicated cases, AGA recommends physicians consider the patient’s history, disease severity and whether they’ve received a high-quality colonoscopy in the past year.
AGA also recommends waiting at least six to eight weeks after an acute episode. Screening before the episode has fully resolved increases risk of perforation, discomfort and can create a more technically demanding procedure for the clinician.
Many different pathologies can mimic diverticulitis symptoms, including ischemic colitis, inflammatory bowel disease and visceral hypersensitivity. The AGA recommends CT scan as the best imaging modality to assess for the presence and severity of diverticular disease.
PREVENTATIVE CARE
While a nutritious diet is a cornerstone of good health for everyone, patients with a history of diverticulitis should be especially mindful of their eating habits.
During the acute phase of uncomplicated diverticulitis, “bowel rest” through a clear liquid diet is advised with a goal of patient comfort. If a patient cannot advance their diet after three to five days, a follow-up appointment should be scheduled immediately.
When returning to solid foods, a vegetarian diet and a simple, high-fiber diet rich in fruits, vegetables, legumes and whole grains are associated with decreased diverticulitis risk. And despite myths, corn, popcorn, berry and nut consumption do not increase risk.
To further reduce risk, physicians should encourage patients to participate in vigorous exercise, stop smoking, maintain a healthy weight (obesity increases risk) and watch alcohol consumption. While drinking alcohol generally is not a risk factor, alcoholism does increase risk. Regular use of nonsteroidal anti-inflammatory drugs (NSAIDs) and opiate analgesics should also be avoided, the report states.
Currently there is no medication available to prevent recurrence of diverticulitis. Although multiple studies have examined rifaximin, probiotics, and 5-aminosalicylic acid (mesalamine) on diverticulitis recurrences, both AGA and ASCRS found insufficient evidence to support their use.
“There seems to be a general consensus that uncomplicated diverticulitis has been historically overtreated,” Dr. Teetor says. “We now have a better understanding of the disease process and a greater focus on inflammation rather than infection. The patient must always be managed as a whole with specific factors taken into account, but trends point toward less use of antibiotics, less emphasis on surgery, all of which brings improved patient outcomes.”
For physician consultation or To refer a patient with suspected diverticulitis, call 216-553-1976.
Reference
Peery AF, Shaukat A, Strate LL, AGA Clinical Practice Update on Medical Management of Colonic Diverticulitis: Expert Review, Gastroenterology (2021), doi: https://doi.org/10.1053/j.gastro.2020.09.059.


